Molecular conversations between cells could explain why allergies develop
There are strong links between disordered gut flora and the development of allergies. But why? Eva Sverremark-Ekström is mapping the communication between bacteria in the gut and immune cells. For example, her research shows that the bacteria appear to send critical messages to the immune system, using nano-sized sacs filled with molecules.

Eva Sverremark-Ekström, professor of immunology at Stockholm University, studied her first immunology course in the early 1990s and, since then, she has been captivated by our immune system, which has an outstanding capacity for defending us from viruses and bacteria.
“It was love at first sight. It was so fascinating to dive into this incredible system that keeps us healthy from when we are born until we die,” she says.
Has linked lactic acid bacteria to a reduced risk of allergies
Her research largely sets out to understand how the immune system develops in interaction with the gut flora. Since the beginning of the 2000s, in collaboration with physicians who collect clinical samples, her research group have made detailed studies of how the gut flora and immune system mature in children with a risk of allergies.
“We have seen – in repeated studies – that the occurrence of some types of gut bacteria are linked to a reduced risk of developing allergies,” she says.
These bacteria are lactic acid bacteria, also called Lactobacilli. When her research group tested transferring a gut flora that is rich in lactic acid bacteria to animals with no microbes in their guts, it had a significant effect on the immune system of the second generation.
“There were quite major differences. Mice who grew up with parents who had lactic acid bacteria in their gut flora had a completely different immunological profile, which can be described as less inflammatory, in comparison to those who had a flora without lactic acid bacteria.
Molecules from lactic acid bacteria have substantial effects on immune cells
To better understand the role lactic acid bacteria play in this allergy drama, her research group cultivate them in the lab. They then expose immune cells, which they have isolated from blood samples from children, to the molecules produced by the bacteria.
“We see very strong effects on the immune cells, which are similar to those we see in animal studies and clinical samples. This is why we believe that Lactobacilli can directly affect the immune cells,” says Eva Sverremark-Ekström.
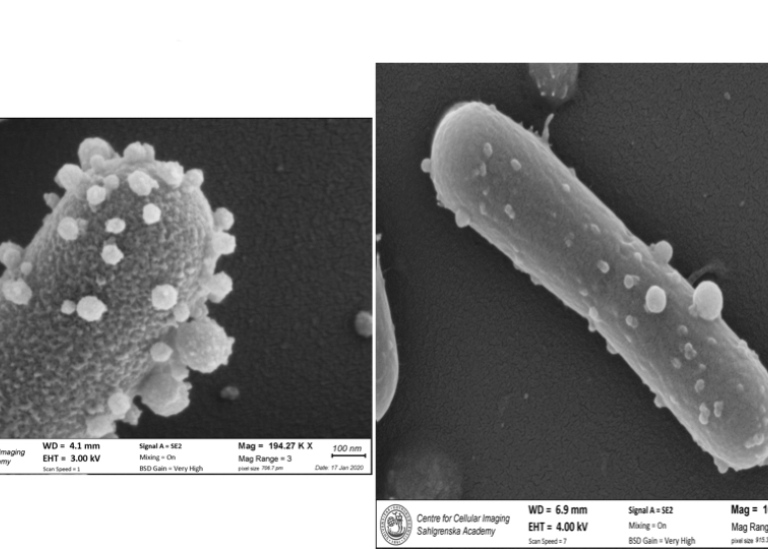
The research group is now conducting detailed studies of the molecular communication between gut bacteria and the immune system, which has led to surprising discoveries. One is that the bacteria appear to send their messages using small sacs they pinch off from their cells. These sacs are called vesicles and seem to carry the bacteria’s messages to the immune cells.
“This is a relatively new field. We know that the vesicles contain remnants of DNA and various proteins, but they have not yet been properly characterised,” says Eva Sverremark-Ekström.
Lactic acid bacteria calm down key players in the immune system
The molecules produced by the lactic acid bacteria also appear to affect dendritic cells, which are vital components in our immune system and can activate other immune cells.
“Lactic acid bacteria seem to be able to reprogramme dendritic cells, so they change the gene expression in a way that is probably less inflammatory,” says Eva Sverremark-Ekström.
The research group’s experiments show that when the dendritic cells are exposed to molecules from lactic acid bacteria, they send out signals that calm down the rest of the immune system, which could partly explain the reduced risk of allergies.
Will study whether peanut allergy can be cured using peanuts
Because lactic acid bacteria appear to prevent allergies, in an ideal world babies could be given some bacteria at birth, to prevent allergies. Unfortunately, it’s not that simple. When researchers have tested giving babies supplementary bacteria, they have not had a great effect.
“It seems as if it is very difficult to get the bacteria to stay in the gut. They remain as long as they are given as supplements, but when you stop giving them they disappear,” says Eva Sverremark-Ekström.
However, research is increasingly indicating that food allergies can be counteracted if young children are introduced to allergenic foods at an early age. Eva Sverremark-Ekström’s research group will therefore contribute to a study that will last several years, trialling a new treatment for small children with peanut allergy. They will be given small amounts of peanut protein, which is gradually increased to slightly larger amounts. The control group must entirely avoid peanut protein. The hope is that the children’s immune system will develop a tolerance to peanuts and the allergy will be cured.
“We will take samples from the children, both blood and gut flora, so we can see how the treatment affects the gut flora and immune system as the children grow and age.”
There are enormous gains to be had if this treatment provides a cure. Eva Sverremark-Ekström also hopes that more detailed knowledge of how the gut flora affects the immune system will provide keys to developing medical teatments that can prevent allergies developing in people at risk of experiencing problems.
Read more on Eva Sverremark-Ekström´s research.
Text: Ann Fredholm
Last updated: February 4, 2022
Source: Communications Office

